The Body & the Jaw

In The Mind & the Jaw we explored why jaw tension is not really a jaw problem. The brain has chosen to hold the jaw in tension for safety. But here’s the thing – it’s not just the jaw being held in tension – it’s the body too. One example being the jaw and hip connection.
Fascia and Jaw Tension – The Body’s Connective Web
When we say the body is held in tension, more accurately it’s the fascia. Every muscle, bone, nerve, and organ in the body is wrapped and connected by fascia — a continuous, adaptable web of connective tissue that links everything together. Tension within that system doesn’t stay neatly contained in one place.
Fascia responds to how we move, breathe, and hold ourselves — as well as to stress, emotion, and nervous system state. When the system feels safe and well-supported, fascia stays supple and responsive. When tension is held for long periods, it gradually becomes less elastic and more resistant to change.
Fascia researcher Thomas Myers demonstrated this with a cadaver dissection that pulled a single, unbroken strip of tissue all the way from the toes to the tongue — one continuous fascial line through the entire body. The jaw sits inside that system. This is why I include the soles of the feet in my jaw treatments — and why it’s worth exploring at home with a foot roller or massage ball, going slowly and lightly. You’re aiming to reassure the brain, not iron out a problem.
When one area is under strain or holding tension for long periods, the system often redistributes that load elsewhere — sometimes into the jaw. You may recognise this in your own experience. Jaw tension often increases when sitting for long periods in a braced or collapsed posture, breathing shallowly, dealing with ongoing stress or fatigue, or recovering from injury elsewhere in the body.
The Jaw and Hip Connection — Why They're More Linked Than You Think
Of all the whole-body connections I explore in clinical practice, the relationship between the hips and the jaw is one of the most significant. There isn’t one single explanation, but there are a few well-established theories worth considering.
Fascial continuity. The fascial networks we’ve just described run directly from the jaw through the neck, trunk, and into the pelvis and hips. Tension doesn’t stay contained — it distributes across connected regions. Research has found that changes at the jaw can directly influence hip range of motion, suggesting the body may organise strain through these shared connective tissue pathways.
Nervous system and protective holding. The vagus nerve — which as we explored in The Mind & the Jaw directly supplies the muscles of mastication — also links the jaw, throat, diaphragm, and pelvic floor. When the nervous system remains in a heightened state, tension may be maintained across all of these areas at once. Research into TMD suggests that chronic jaw pain is linked to broader nervous system responses rather than a purely local problem.
Whole-body stress and load. The jaw and the hips are both places where people commonly brace and hold under pressure. Studies have observed wider changes in posture and musculoskeletal function when jaw position changes — suggesting that jaw and hip tension may sometimes be different expressions of the same underlying load, physical, emotional, or both.
What I See in Practice — Jane's Story
I want to share an example that illustrates the jaw and hip connection clearly. It relates to my case study during training with Helen Baker at TMJ Massage Therapies.
Jane (not her real name) had lived with jaw problems since childhood. When we worked together she was in her mid-sixties, with a history that included traumatic jaw realignment as a child, several whiplash injuries, and decades of clenching.
We had already made some progress together, but she still felt her jaw was restricted and her bite was off. Something wasn’t shifting.
When we focused on the hips, something changed instantly. Jane noticed a clear release on the left side of her jaw while I was working on her left glute medius — a hip muscle with no obvious connection to the jaw. Later in the same session, during intraoral work to the lateral pterygoid (a chewing muscle) she described an unexpected sense of opening in her pelvis.
A few days later she got in touch. She could open her mouth wider than three fingers for the first time in her life. Walking felt different. Chewing was easier. Her jaw felt softer than she could remember.
The hips hadn’t fixed the jaw. But addressing the hips had created the conditions where the jaw felt safe enough to release.
What This Means in Practice
Whether exploring the jaw and hip connection or other parts of the body, fascia responds best to curious, considered input — not to aggressive pressure or forced movement. The tissue isn’t waiting to be overcome — it’s waiting to feel safe.
In the Jaw Care section we explore how to work with the body and fascia practically — whole-body approaches that create the conditions where the jaw can genuinely let go.
This is Part 4 of 4 in the Jaw Knowledge Series.
Previously: The Mind & the Jaw
Return to the beginning: What TMJ/TMD Really Is
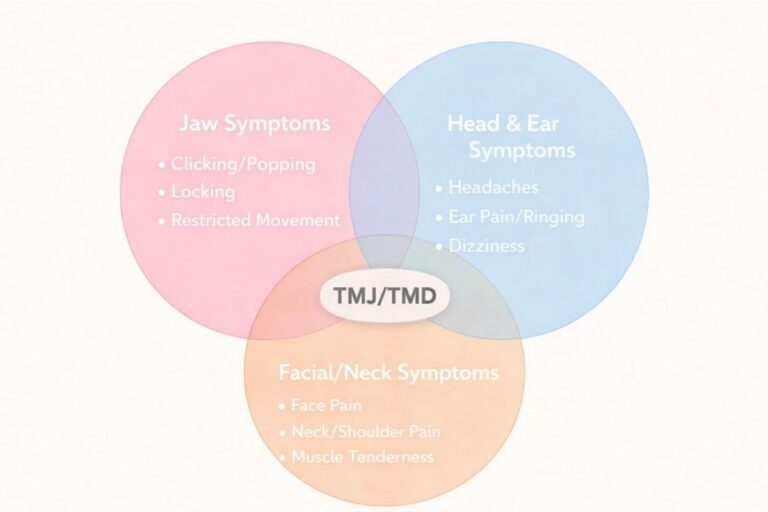
What TMJ / TMD Really Is
TMJ and TMD can sound serious, but is it really? Find out what it means and how it differs from one person to another.
You May Find These Guides Helpful
Looking for something else?
When to Seek Medical Advice
Most jaw tension and TMD symptoms are related to muscle guarding, stress, or nervous-system patterns, and they often improve well with gentle self-care.
It’s a good idea to seek medical advice if you experience:
sudden, severe, or unexplained facial or jaw pain
injury, swelling, or suspected dislocation
numbness, weakness, or changes in vision or speech
a fever, illness, or signs of infection
new pain accompanied by weight loss or general unwellness
persistent symptoms that worry you or don’t improve over time
These situations aren’t common, but it’s always appropriate to check in with a qualified medical professional if something feels unusual or concerning for you.