What TMJ / TMD Really Is
“You have TMJ.” That’s what you have been told, or suspect. You may also have been told it’s TMD. You’re likely concerned. Is it serious? How long will this last? Is this what I’m stuck with?
Straight up — I know it sounds serious and clinical and probably feels unchangeable, but as a TMJ therapist who works with jaw tension clients every day, I assure you: it is rarely serious.
With the right knowledge and approach, most people find they can reduce their symptoms considerably, if not completely resolve them — whether that’s through self-care, professional support, or a combination of both.
What is TMJ? TMJ stands for temporomandibular joint — the joint that connects the jaw to the skull.
What is TMD? TMD stands for temporomandibular disorder, a broad term used to describe symptoms affecting the jaw joint, muscles, and surrounding tissues.
In practice, TMJ and TMD are often used interchangeably. They don’t point to a single cause, diagnosis, or structural problem. They simply describe a pattern of symptoms that can arise for many different reasons — and that pattern looks different in almost every person I work with.
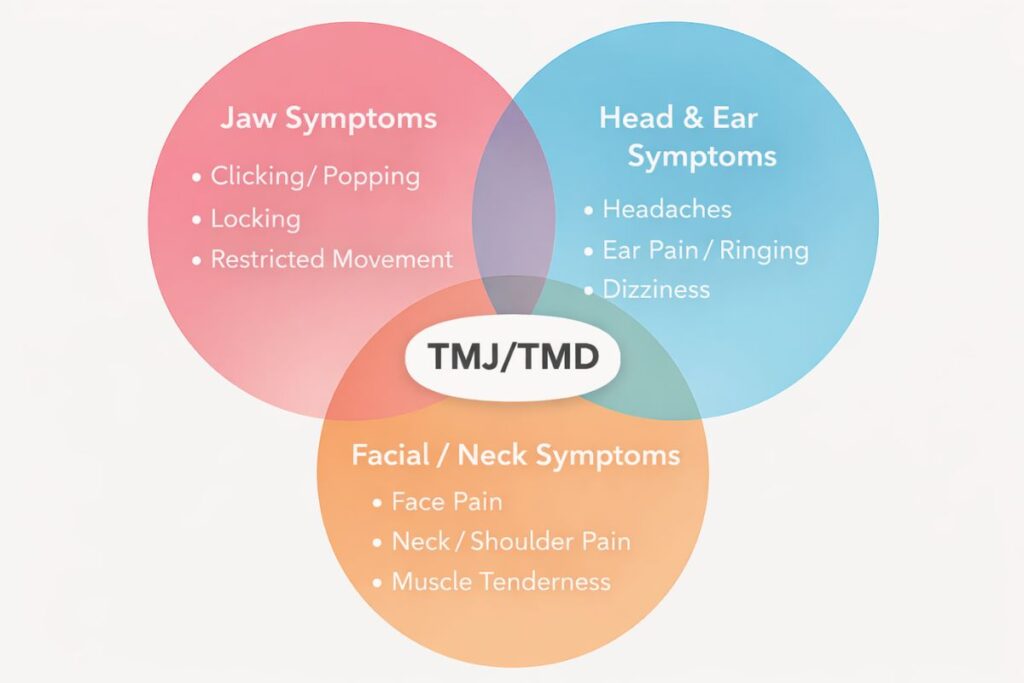
What are TMJ / TMD Symptoms?
TMJ / TMD symptoms vary widely from person to person.
Some people notice clicking or popping without any pain. Others experience tightness, headaches, ear symptoms, or difficulty opening the mouth comfortably. Many people have several of these at once — and find that symptoms shift or change over time.
This variation exists because jaw symptoms are rarely caused by one single factor. Muscle tension, nervous system sensitivity, habits, stress, posture, and past experiences can all influence how symptoms show up.
Two people may have the same label, but very different underlying patterns. This is why there is no single right treatment for everyone with TMJ / TMD — and why approaches that treat everyone the same so often fall short.
Is TMD Serious?
In most cases, no — and this is probably the most important thing I can share with you.
TMJ / TMD is not usually a sign of serious joint disease, structural damage, or something progressively going wrong inside the jaw. It is far more often related to how muscles, connective tissue, and the nervous system are responding to load, stress, habits, and past experiences.
This is also why imaging can often be unhelpful or misleading. Scans frequently show findings that sound concerning but are just as common in people with no jaw symptoms whatsoever. A scan that looks unusual doesn’t necessarily explain the cause of pain — and it certainly doesn’t mean things can’t improve.
This is why there is growing concern that musculoskeletal conditions like TMD can become overmedicalised — meaning medical intervention isn’t supported by clinical evidence.
Interestingly, NICE, the body that sets clinical guidelines for the NHS, recommends that for most people with TMD, the first approach should be education, and self-management and that conservative and informed approaches frequently outperform medical intervention.
Hopefully that has given you a foundation of what TMJ/TMD is. A next logical question may be why it is happening?
The following articles explore that in more depth — what tends to cause jaw tension to persist, how the nervous system and mind play a role, and how the body as a whole is involved.
This is Part 1 of 4 in the Jaw Knowledge Series.
Next in the series: Causes of Jaw Tension
Causes of Jaw Tension
What causes TMD? Why do jaw issues begin? As a TMJ therapist, here are the 3 clear categories I see in my clinic.
You May Find These Guides Helpful
Looking for something else?
When to Seek Medical Advice
Most jaw tension and TMD symptoms are related to muscle guarding, stress, or nervous-system patterns, and they often improve well with gentle self-care.
It’s a good idea to seek medical advice if you experience:
sudden, severe, or unexplained facial or jaw pain
injury, swelling, or suspected dislocation
numbness, weakness, or changes in vision or speech
a fever, illness, or signs of infection
new pain accompanied by weight loss or general unwellness
persistent symptoms that worry you or don’t improve over time
These situations aren’t common, but it’s always appropriate to check in with a qualified medical professional if something feels unusual or concerning for you.

